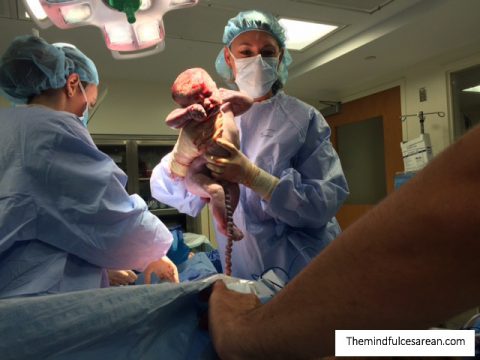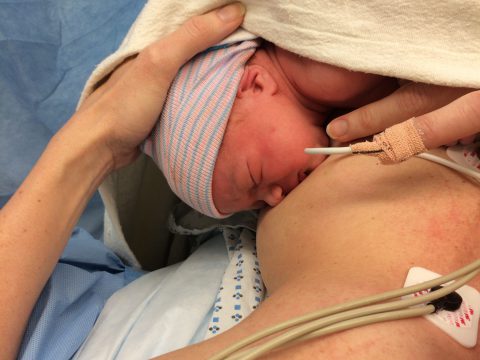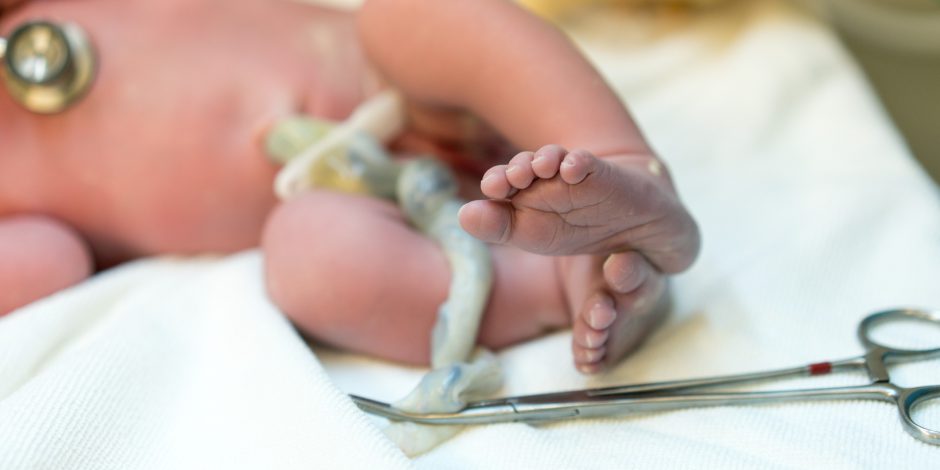
In most cases, delayed cord clamping is possible with a cesarean. Ask your doctors to place the baby on your chest or thighs and wait to cut the cord 30 to 60 seconds. It might help to remind doctors that the American College of Obstetrics and Gynecology now recommends delayed cord clamping, even with a cesarean.
Why ask for delayed cord clamping?
In utero, the cord is an essential part of a baby’s circulatory system. When the newborn emerges at birth, the cord— almost finished with its work, but not quite— transports a significant amount of the baby’s total blood volume from placenta and cord to the baby’s body.(i) The placental transfusion moves a volume of iron-rich red blood cells, immunologically important white blood cells, and, perhaps most important of all, pluripotent stem cells to aid the development of immature organs.(ii) The oxygen-rich blood also provides a secondary source of oxygen at the delicate time of transition from gas/cord oxygenation to lung breathing. Studies are currently demonstrating that what happens in the minutes following the birth of a human may have an impact on the baby’s health for years to come, especially if that baby is a boy.(iii)
Delayed Cord Clamping: The American College of Obstetrics and Gynecology
In a strongly worded editorial published in ACOG’s Journal Obstetrics and Gynecology, Dr. Ryan McAdams recommends that babies should receive delayed cord clamping no matter if they are born vaginally or by cesarean. With a cesarean he says babies can be held on the mother’s thighs above the level of the uterus while waiting two to three minutes to clamp the umbilical cord.
Dr. McAdams writes, “In term neonates, delayed cord clamping has been associated with decreased iron-deficient anemia and increased iron stores with potential valuable effects that extend beyond the newborn period, including improvements in long-term neurodevelopment.” He cautions that, “Failure to adopt beneficial practices, especially evidence-based ones, may constitute unnecessary harm. Reluctance to implement delayed cord clamping nationally may place thousands of children born this year at unnecessary risk for neurodevelopmental delays, cerebral palsy, and behavior problems.” He concludes, “For those privileged enough to participate in the birth of neonates, there is a need for increased appreciation and awareness of which precious minutes may count most.”(iv)
In January, 2017 ACOG issued a statement recommending a 30 to 60 second delay in cord clamping for both vigorous preterm and term infants, no matter their mode of delivery. In the case of cesareans, the committee suggests the newborn can be “placed on the maternal abdomen or legs or held by the surgeon or assistant at close to the level of the placenta until the umbilical cord is clamped.”(v)
Who Else Recommends Delayed Cord Clamping? Most Everyone!
- The World Health Organization recommends that the umbilical cord not be clamped earlier than 1 minute after birth in term or preterm infants who do not require positive pressure ventilation.
- Neonatal Resuscitation Program guidelines from the American Academy of Pediatrics recommend delayed umbilical cord clamping for at least 30–60 seconds for most vigorous term and preterm infants.
- The Royal College of Obstetricians and Gynaecologists recommends deferring umbilical cord clamping for healthy term and preterm infants for at least 2 minutes after birth.
- The American College of Nurse–Midwives recommends delayed umbilical cord clamping for term and preterm infants for 2–5 minutes after birth.”(vi)
Milking the Cord?
When doctors feel 30 to 60 seconds is too long a period to wait to clamp the cord (if the baby needs to be resuscitated and they lack a surface on which to simultaneously resuscitate and keep the cord intact, for instance), they can hurry the placental transfusion by milking (or stripping) the cord. Milking the cord allows the baby to receive a significant amount of cord blood in 10 to 15 seconds. The practice of milking the cord is currently being studied. ACOG says that as of January, 2107, “there is insufficient evidence to either support or refute umbilical cord milking in term or preterm infants.”(vii) Discuss this possibility with your doctor.
“As she slowly pulled him out, at my request, the anesthesiologist lowered the sheet so I could watch. He kept saying it was unhygienic to lower the sheet, but I kept reminding him that it was fine, and that my doctor had okayed it. Also at my request, my doctor milked the umbilical cord for 30 seconds (as long as she felt medically comfortable doing, given my complications), so my baby would benefit from the extra blood volume.” Athena Reich
The Operating Room Needs a New Table
The table to which most babies born by cesarean will be taken is usually about 10 feet from the mother, close enough for the mother to hear her baby and feel reassured, but much too far for the umbilical cord to reach. The warmer, as this table is known, is a product of its time, reflecting twentieth century obstetrical beliefs and practices. Hospitals are now in need of a new, movable table in every delivery and operating room that reflects our growing twenty-first century understanding of the importance of keeping mother and baby connected for the first few minutes after birth, even when a baby is born with meconium and might require suctioning, even when a baby might be slow to start breathing and need assistance, even when a baby is born by cesarean.
The Inditerm Company based in the U.K. has designed a mobile table that facilitates access to a baby for resuscitation or other care while leaving the cord intact. On their website, they note that doctors currently have to chose between resuscitation and delayed cord clamping.(viii) The table’s mobility means a baby can receive the placental transfusion while simultaneously benefiting from any necessary suctioning, resuscitation efforts, or other procedures. Ask if your hospital offers such a table, sometimes known as a birth trolley.
Ask!
Most doctors have performed cesareans for years where as soon as the baby is born they have immediately clamped and cut the baby’s cord and handed the baby over to the pediatrician. This has been routine for midwives and nurses as well. The 2017 ACOG guidelines recommending delayed cord clamping (and the abundance of research behind those guidelines) is pushing many practitioners to adopt new practices when it comes to cesarean delivery. Ask your doctors how they are incorporating the 2017 guidelines. Ask your midwives too! Ask everyone involved in your care!
I was on a birth where an induction led to a cesarean. As we were preparing to go to the operating room, the couple asked their midwife if they could delay cord clamping with a cesarean. “No,” she answered, “I’m sorry. With a cesarean, the pediatrician needs to take the baby right away to the warmer.” After she left the room, the doctor who was to perform the cesarean entered the room to say hello. I motioned to the father, suggesting he ask one more time for delayed cord clamping. They repeated their question and the doctor was very positive about the idea. She said she would gladly honor their request for delayed cord clamping if at all possible. My clients were thrilled to hear it. As it happened, the baby was born in great shape and received delayed cord clamping simply because his parents had asked a second time. You just never know.
(i) Farrar D, Airey R, Law G, Tuffnell D, Cattle B, Duley L., “Measuring placental transfusion for term births: weighing babies with cord intact,” BJOG 18(1) (2011):70–75. Retrieved at http://onlinelibrary.wiley.com/doi/10.1111/j.1471-0528.2010.02781.x
(ii) Tolosa, J., Park DH., Eve, D., Klasko, S., Borlongan, C., & Sandberg, P., ”Mankind’s first natural stem cell transplant,” J. Cell. Mol. Med. 14(3) (2010): 488-495
(iii) Andersson, O., Lindquist, B., Lindgren, M., Stjernqvist, K., Domellöf, M., & Hellström-Westas, L. “Effect of Delayed Cord Clamping on Neurodevelopment at 4 Years of Age,” JAMA Pediatr (2015): 631-631. doi: 10.1001/jamapediatrics.2015.0358
(iv) McAdams, R. “Time to Implement Delayed Cord Clamping,” Obstetrics and Gynecology, 123(3)(2013)
(v)Maria A. Mascola, T. Flint Porter, Tamara Tin-May Chao, “Committee Opinion: Delayed Cord Clamping After Birth,” The American College of Obstetrics and Gynecology, Number 684, January 2017. Retrieved at http://www.acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-Obstetric-Practice/Delayed-Umbilical-Cord-Clamping-After-Birth
(vi) Mascola, “Committee Opinion: Delayed Cord Clamping After Birth,” January, 2017.
(vii)Mascola, “Committee Opinion: Delayed Cord Clamping After Birth,” January, 2017.
(viii) Inditherm Neonatal Resuscitation (Lifestart)
http://www.inditherm.co.uk/medical/neonatal-resuscitation-lifestart/